COMMUNICATION
Communication is made up of skills that many of us take for granted. We use our words, tone of voice and body language to send messages to each other.
As people age, they can develop illnesses or impairments. These losses affect a person’s ability to communicate well with the people around them. Our role is to deliver and receive messages clearly, simply, and accurately.
It is important that, as workers, we can connect and communicate with the older people in meaningful ways. Our role is to help others to make decisions, understand their choices and safeguard the dignity of the individual.
In this module we will look at:
- What communication is and the elements that make up communication
- What skills are important for effective communication
- The common barriers to communication for older people
- Strategies for important conversations
To effectively communicate, we must realize that we are all different in the way we perceive the world and use this understanding as a guide to our communication with others.
– Tony Robins
Standards Mapping
Click the coloured headings below to view how the content in this lesson correlates with the Aged Care and National Disability Service Standards:
Aged Care Standards
- Each consumer is supported to exercise choice and independence and communicate their decisions
- Workers communicate respectfully and recognise and respect a consumer’s individuality in all aspects of care and services
- The workforce can describe different ways information is communicated to make sure it’s easy to understand and accessible to diverse consumers
- Workers listen to what the consumer wants
- Relevant risks to a consumer’s safety, health and well-being are observed and managed
- The outcomes of assessment and planning are effectively communicated to the consumer
- Services and supports for daily living assist each consumer to have social and personal relationships
- Deterioration or change of a consumer’s mental health, cognitive or physical function, capacity or condition is recognised and responded to in a timely manner
- Workers are aware of when to utilise an interpreter vs. a bilingual worker
- Consumers are aware of their right to communicate in their preferred language
- The workforce is recruited, trained, equipped and supported to deliver the outcomes required by these standards
- Workforce interactions with consumers are kind, caring and respectful
- Good information management systems mean the consumer does not have to keep repeating their story
For more information see the Aged Care Standards. You can also download the Aged Care Standards in languages other than English.
Disability Service Standards
- The service supports active decision-making and individual choice including the timely provision of information in appropriate formats
- The service works together with an individual to identify their strengths, needs and life goals
- The service provides accessible information in a range of formats
- The service monitors and addresses potential barriers to access
- The service uses person-centred approaches including the active involvement of people with disability, families, friends, carers and advocates to review policies, practices, procedures and service provision
For more information see DACSSA’s page on the National Standards for Disability Services. You can also download the National Standards for Disability Services in languages other than English.
Elements of Communication
Communication often comes naturally to humans. We learn from an early age how to interact with others in a way that gets our needs met. We do this long before we learn to speak. Our words only make up part of the message we send and receive.
Our message is communicated and received according to three elements. See the image below.
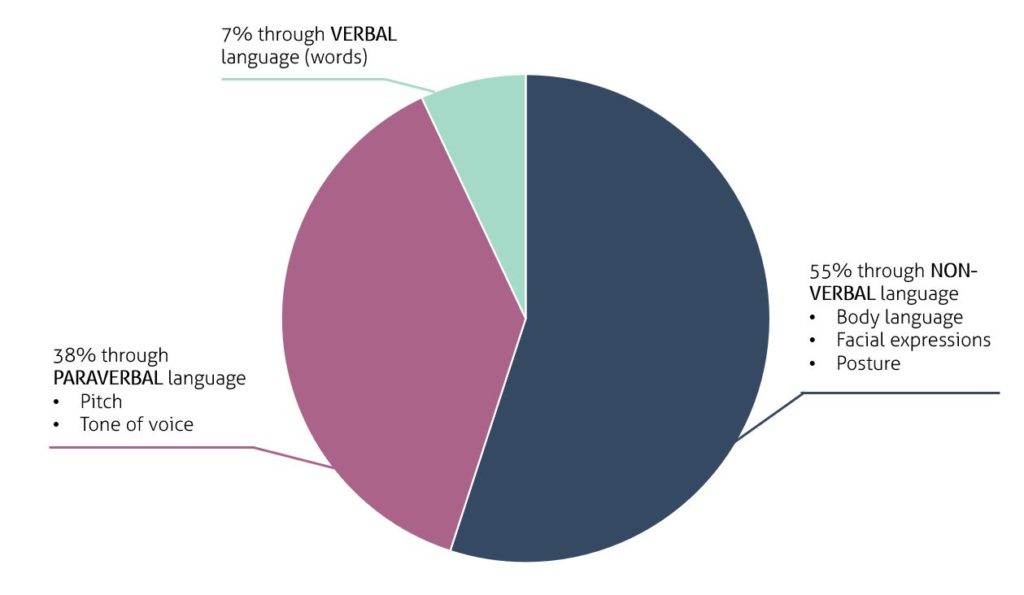
Click the tabs below to learn more about these three elements of communication.
Although the words we use only make up 7% of the meaning of our message, they are still important. Abusive and offensive language at work will always be inappropriate no matter the paraverbal or non-verbal cues you use. However, there is more subtle language that can affect the way your message is perceived.
For example, refer to the people you work with by their name. Calling the people we work with ‘dear,’ ‘love’ or other terms of endearment may seem sweet but it can come across as disrespectful and demeaning. Be sure you know the preferred name of the people you work with and use it.
Be aware of the language that others do or do not use. Using jargon or colloquialisms might confuse some people and not others. For example, you can use technical terminology when speaking to colleagues but avoid this with the people you care for. Keep in mind that everybody has a different background and level of knowledge.
To make sure that your carefully selected words are sending the right message, you must also make sure your paraverbal and non-verbal cues match the message.
Paraverbal language is about how we say our words. This makes up for 38% of the meaning of our message. Paraverbal language can include a number of elements. It can include:
- The pitch – whether our voice is high, low or changes
- The pauses between words
- How quickly we speak
- The words we emphasise
- The volume we use
If you are interested in learning more about tone, view this video.
Take a moment to reflect on what your tone of voice sounds like. If you aren’t sure you could ask someone you know well that will be honest with you.
Then think about how your tone of voice might be perceived by others. If your tone of voice makes you sound like you are busy or frustrated this may make you less approachable. If your tone is always happy you might find people shy away from speaking to you about difficult topics.
It is important that our tone of voice fits with the message that we are trying to communicate. For example, if we are trying to reassure someone we cannot sound frustrated or annoyed.
Finally, our non-verbal cues communicate 55% of the meaning of our message. Non-verbal cues include:
- Facial expressions – frowning, smiling, raising an eyebrow
- Gestures – pointing, giving thumbs up, using eyebrows to point to a place or person
- Posture – standing straight, arms crossed, leaning against a wall
- Eye contact
- Touch
- Space between you and someone else
Non-verbal communications means that people do not have to use language or words to communicate. Communication without words can be more challenging to a person inexperienced in how to understand and share information when people communicate non-verbally.
Hover over or click the cards below for some examples of how we can incorporate this knowledge into our work.
Verbal
Tone
Facial Expressions
Body Language
A Moment of Reflection...
Think of a time when the words you were saying and your body language or paralinguistics did not match.
How do you think your message was received?
When the eyes say one thing, and the tongue another, a practiced man relies on the language of the first.
– Ralph Waldo Emerson
Communication Skills
Active Listening
Listening is about more than hearing the words that a person is saying. It is also about reading their non-verbal cues. But most importantly it is about understanding their point of view – their beliefs, their thoughts, their emotions. If we can do this, we may gain important information, learn something new or improve a relationship.
To do this we need to focus on the speaker and what they are really trying to say. We must listen actively. Watch the video below for some tips on active listening.
Open questions help us to improve the information we receive.
Closed questions mean that the person answering can only answer with ‘yes’ or ‘no’ or words that have been chosen by the questioner. Too many closed questions in a row can start to sound (and feel) like an interrogation! Closed questions are useful for clarifying and fact checking but keep the control of the conversation with the person asking the questions.
Open questions usually start with the words ‘what, why and how.’ They allow the person who is answering the question to give a detailed answer. This might be facts, information or emotions and thoughts.
Look at the questions below. The questions are asking for the same information, but the open questions allow the conversation to flow.
open questions
- How are you feeling today?
- Tell me about your family.
- What would you like to drink?
- How was your day?
- How are you feeling about...
closed questions
- Are you feeling okay today?
- Do you have any children?
- Do you want tea or coffee?
- Did you have a good day?
- Are you feeling angry/tired/nervous?
Active listening does not come naturally to us, but it will improve all relationships, not just those at work. Some elements might be easier for us than others. We must practice daily!
When we listen to others they feel heard, we build rapport, trust and connection. When we listen to others they are more likely to want to listen to us in return.
Active Listening
VERBAL
- Ask open questions
- Make affirmative sounds
- Allow for silence
- Avoid interrupting
NON-VERBAL
- Face the talker
- Mirror eye contact
- Open body posture
- Nodding
- Notice their non-verbal communication
RESPOND
- Ask open follow up questions
- Paraphrase or summarise
- Avoid giving advice
- React with facial expressions
STAY FOCUSED
- Let the talker talk
- Resist the temptation to make it about you
- Listen without planning your response
- Avoid distractions
A Moment of Reflection...
Look at the elements of active listening above.
- Which do you think you are good at already?
- What could you afford to practice more?
We have two ears and one mouth so that we can listen twice as much as we speak.
– Epictetus
Empathy and Validation
Paraphrasing and summarising while actively listening will promote empathy and validation. Empathy is different to sympathy, view the video below for more information.
Empathy is important for everyone but especially for vulnerable people who may be socially isolated.
Validation is similar in practice to empathy. Validation means letting a person know that what they think, believe or feel has been acknowledged. We do not have to agree with their experience, but we do need to let them know they have been heard. If we are not validating a person’s experience we are being invalidating. Invalidation is rejecting or dismissing the way a person feels or what they believe.
Older people we work with can act out with difficult behaviours and challenging attitudes when they are unable to communicate what they want. Due to their losses, (physical, mental, social, emotional) we can start to see the person as the problem. We should see the situation as the problem. The older person may feel frustration, sadness, anger or fear. To communicate with these emotions is difficult. Our role is to let them know we are trying to understand what they are experiencing, needing or feeling. If we validate their feelings with kindness, we are demonstrating empathy.
Look at the examples of validation and invalidation in the image below.
Click to view in full screen.
A Moment of Reflection...
- Think of a time when you had your emotions or thoughts dismissed (invalidated). How did it feel?
- Think about a time when your emotions or thoughts were understood by someone else (validated). How did it feel?
- How can you practice validation with the people you work with?
Empathy is seeing with the eyes of another, listening with the ears of another and feeling with the heart of another.
– Alfred Adler
Communication Barriers
Many of us take communication for granted. There are many barriers to communication. Some we might experience daily. For example, a very noisy room or a text message instead of a face-to-face conversation. There are many people who struggle with communication on a day-to-day basis.
Older people and people with a disability are some of these groups that are more likely to have trouble communicating.
Impairments of communication do not mean the person cannot communicate at all. We must be aware of the needs of the people that we are supporting. With this knowledge we can help them to overcome these barriers.
Click the tabs below to explore some common barriers to communication and how we can reduce them.
Bright lights, dim lights and noisy rooms make communication difficult. They can lead to the receiver of the message not hearing the verbal cues or seeing the non-verbal cues. As we know, both are very important for receiving a message.
Some people have different sensory needs and may need a brighter or darker room to effectively receive a message. Similarly, some people will struggle to hear if there is background noise like music or another conversation.
We can reduce these barriers by:
- Turning lights on or off
- Closing or opening curtains
- Turning music or TV off
- Moving away from noisy spaces
As we age we can gradually lose our hearing. Sometime people lose their hearing due to trauma or illness.
People can have partial or full hearing loss. Some people cannot hear anything. Others will be able to hear some words and sounds.
Sometimes people will use hearing aids to improve their ability to hear. This does not mean that their hearing is normal with the hearing aid. It means that their hearing is better than what it would be without the hearing aids.
We can reduce this barrier by:
- Reducing background noise for people with partial hearing loss
- Using gestures or touch to get their attention
- Encouraging the use of hearing aids for partial hearing loss
- Letting the person see our face as we speak so that they can lip read and see our facial expression
As we age we can gradually lose our ability to see. Some people also lose their sight due to trauma or illness.
Like hearing loss, we can lose our sight a little or a lot. Some people cannot see anything at all. Some will be able to see as if they are looking through a fog. Glasses or contact lenses can help with partial sight loss.
We can reduce this barrier by:
- Encouraging the use of glasses or contact lenses if appropriate
- Managing the amount of light in the room
- Magnifying words and images
- Describing options
People lose their ability to speak due to trauma, cognitive impairment, stroke and other illnesses. Speech impairment might be because of loss of muscle movement, brain injury or nerve damage. Some disabilities or illnesses may stop the person from learning to speak at all and some may cause them to lose the ability over time.
We can reduce this barrier by:
- Allowing the person time to communicate
- Using alternative communication – writing down what they need, giving them options to read
- Sign language using specific hand gestures
- Using images and symbols to communicate (like these pictures)
Some disabilities and illnesses can cause cognitive impairment. This means that the person’s brain does not work in a way that it is expected to. This could be because of a brain injury but in aged care we see dementia or Alzheimer’s Disease as a common cause.
Cognitive impairment looks different for everyone. It might result in the difficulty of hearing, sight, speech, thought or movement.
In the early stages of dementia, people may have trouble coming up with the right name for a person or word for an object. As they enter the later stages of their condition, they may speak less and less.
We may have to use a range of strategies to reduce these barriers individually. Some general strategies include:
- Getting to know the persons likes & dislikes
- Include the person in discussions about them respectfully
- Position yourself at their level and make eye contact
- Use simpler, more direct sentences, one question at a time
- Giving them more time to respond
The language we use to communicate is important. If someone sends us a message in a language we do not speak we will not receive it well. We can still read the tone and the body language but the words will not be understood.
Culture also affects the way that we communicate. For example, in Australian culture it is disrespectful to not make eye contact with someone who is speaking. In other cultures, making eye contact with elders is seen as disrespectful.
All cultures have cultural taboos. These are topics that are not usually discussed due to shame or privacy. For example, in Australia it is rude to ask how much money a person makes or their weight. Other cultures would not approve of discussions about sex or death.
We can reduce this barrier by:
- Using simple language and gestures
- Knowing key words or phrases in the person’s preferred language (e.g. toilet, drink or pain)
- Having a bilingual worker (someone who speaks more than one language) translate
- Using a qualified interpreter when needed for legal or health matters – it’s really important that the person understands everything being said
- Checking your understanding of what they have said
- Checking their understanding of what you have said – ask them to repeat it back in their own words
- Having open discussions about cultural differences
- Being aware of cultural taboos
A Moment of Reflection...
- What communication barriers are experienced by the people you work with?
- How can you help them to send their message more clearly?
- How can you help them to receive a message more clearly?
In the last section we talked about barriers to communication caused by impairments and physical barriers. There are also interpersonal barriers to communication. These are barriers that happen due to a person’s beliefs or behaviours. Some interpersonal barriers to communication may include:

- Disrespect
- Blame
- Making assumptions
- Failure to ask appropriate questions
- The desire to be right
- Focusing on the past or future rather than the present moment
It is important for us to be able to identify when these barriers are happening for us and for the people we work with. These barriers cause us to be closed to communication. We may unconsciously choose to ignore verbal and non-verbal cues. They cause us to be invalidating and we fail to show empathy. These barriers will weaken relationships and we will fail to provide much needed supports to our clients.
Practicing active listening and asking open questions will help us to overcome these barriers. Self-awareness of our own beliefs, behaviours and attitudes will also help to reduce these barriers.
A Moment of Reflection...
Think of a conversation when you have been affected by an interpersonal communication barrier, e.g. disrespect, blame.
- What happened? What was the result of the conversation?
- How would the situation have been different if the barrier was identified and reduced?


Case Study - Joe
Joe is a man in his 80’s. He has always been an active man. Migrating from Italy in the 1950’s as a teenager. He helped his mother start a dry-cleaning business. He also worked driving trucks and in his free time built their house and market garden in the Western Suburbs of Adelaide.
He now lives in residential care due to the physical health setbacks he has experienced from such hard physical labour as a younger person. He has limited mobility, depression and short-term memory loss. He can be grumpy and ignores staff when he is unhappy.
When Joe’s extended family members visit, he is animated and chats with them about his life. He is interested in their work and gardens. He plays an Italian card game with his grandson. They laugh and exclaim in Italian. They sometimes bring fruit or produce from their gardens or gelati in a cup for Joe. He proudly tells staff about these visits. He becomes withdrawn again quickly after the visit.
Case Study Reflection...
- What are some of the barriers that prevent Joe from communicating well?
- How can staff communicate with Joe to reduce his bad mood?
- What could staff try to help Joe be more conversational?
- What type of questions might open conversations with Joe?
- What interests could staff talk to Joe about?
- Knowing Joe’s valued roles, like relationship and work roles, can create more meaningful conversations. What else could you ask Joe about?
COMMUNICATION IS ONLY EFFECTIVE WHEN WE COMMUNICATE IN A WAY THAT IS MEANINGFUL TO THE RECIPIENT, NOT OURSELVES.
– Rich Simmonds
Important Conversations
We have conversations with the people we work with every day. Sometimes we have to have important conversations. Important conversations include discussions about changes to support, illness and death. We may need to have these conversations with the client or their families. This can be uncomfortable for everyone involved but it is better to have them sooner rather than later.
Important conversations can become difficult conversations. Difficult conversations can have poor outcomes if they are not managed correctly. An important conversation may become difficult if any of the following are involved (click the arrows below to view all slides):
It is easier to manage emotions and behaviours if we understand what can make an important conversation difficult. For example, if we are frustrated with the behaviour of someone else. Before we speak to that person, we need to centre ourselves. We need to make sure our own emotions are not going to affect our behaviour and escalate the situation. This can take a lot of practice!
Thankfully, there are some tips we can use to help prepare us for these conversations. When we prepare for an important or difficult conversation it is more likely there will be a positive outcome – for us, our client and their family.
Prepare yourself for the conversation. Make sure you a ready emotionally and that you have the right information
Choose an suitable time and place for the discussion. You will need to consider the person’s communication needs and their privacy. Be aware of any communication barriers and cultural needs.
Also consider if anyone else may need to be present, e.g. family member, health professional, interpreter.
You may want to plan general dot points of conversation but do not write a script. Scripts make conversations one-way and do not allow for the other person to respond.
Be aware of culturally appropriate behaviour. Be sure that your eye contact, how close you sit and how you broach the subject is in line with cultural needs.
Give the person your whole attention – avoid taking notes or using devices.
Ask the person if now is a suitable time and give them a warning that an important conversation is about to occur, e.g. “Hey, Jerry. Is now a good time to talk about toileting? I’ve noticed it’s been difficult for you to get to the bathroom on time lately.“
Relate to the person. Use your active listening skills to show empathy, care and compassion, e.g. “I know it can be embarrassing and frustrating, but incontinence happens to a lot of us as we get older. Let’s think of some ways that we can make this easier for you.“
Find out what the person already knows, e.g. “What do you already know about incontinence?” Their answer will help you continue using similar language and fill in the knowledge gaps for them.
Use understandable language or alternative communication. Remember that some people receive messages better with aids like signing or writing.
Give small chunks of information at a time and be prepared to repeat these. If this is a difficult conversation for the person receiving the message they might take a little while to understand. Go at their pace.
Validate thoughts and emotions, e.g, “Jerry, I can see this is really upsetting for you.”
Allow time for silence. Let the information sink in. Let the person think about how they are feeling and how to respond.
Reassure the person but do not lie or be dishonest about outcomes.
Check for understanding often, e.g. “Does that make sense?” You could ask the person to repeat back small sections in their own words to make sure they have understood.
Ask the person if there is anything that you or the organisation can do to help them, e.g. “Do you need me or another worker to help you speak to your doctor?“
Make sure the person has understood what you have told them. Summarise the conversation in a sentence or two including where we go from here.
Be open to questions. Also make sure you are okay with saying you do not know the answer to some questions. Let the person know you will follow up and get back to them as soon as possible.
Do not give personal opinions or information where you are not qualified to do so.
Suggest a time for follow up so that they can ask further questions and you can give any extra information.
Leaving the person with pamphlets or information in a different format may be helpful.
Follow up on answering questions you could not answer. Provide this information to the person as soon as possible.
Document the conversation.
Attend any follow ups if they have been arranged.
Reflect on how the conversation went. What went well? Were there extra communication or interpersonal barriers that you did not expect? What could be done better next time?
Debrief with a supervisor or colleague to help you reflect better on the situation.
Conclusion
Communication is something that many of us take for granted. The way that we communicate with the people we work with can make or break their day. Our communication is important in promoting wellbeing for clients.
The words we use are important but our non-verbal communication says the most. We need to make sure that our words, our tone and our body language all match the message we are sending.
Active listening can help us to show empathy and validation to the people we work with. These are skills that we learn with practice. They are valuable in our work and personal relationships. These skills help us to build rapport and make others feel valued.
Important conversations can become difficult conversations when emotions are high or knowledge is low. It is crucial that we plan for these to get good outcomes.
Further Resources
The content below are resources that you can access if you are interested in getting more information. Click the topic you are interested in for links to videos, articles and activities.
Video: The Importance of Non-Verbal Cues as Told by Friends, Kimberley Klawans, YouTube
Article: Active Listening – MindTools
Video: The Power of Listening – William Ury, TedXSanDiego, YouTube
Video: 5 Ways to Listen Better – Julian Treasure
Fact Sheet: Caring for Someone with Dementia – Dementia Australia
Fact Sheet: Interpreters: An Introduction, Centre for Culture, Ethnicity and Health
Video: Hints and Tips for Working with Interpreters, Australian Department of Home Affairs
FREE Online: Ageing in Australia: The Immigrant Experience video, Centre for Cultural Diversity in Ageing
FREE Online: Effective Communication Techniques, Carer Gateway
FREE Online: Talk to Us First, Older Persons Advocacy Network




